
The Microbiome Functions and Functional Medicine Part: 1 El Paso, Texas
The microbiomes in our bodies are fascinating. They help our various organs function correctly, helping out our immune systems battle terrible stuff. They can tell us what we are doing to our bodies when we consume food. However, the microbiomes in our gut tell us a different story as we are going to discuss what does microbiomes do as it functions in our body as well as our gut.
The relationship between the gut microbiota and its host plays a crucial role in:
- immune system maturation
- food digestion
- drug metabolism
- detoxification
- vitamin production
- prevention of pathogenic bacterial adhesion
Also, the composition of the microbiota is influenced by environmental factors such as diet, antibiotic therapy, and environmental exposure to microorganisms.
Table of Contents
Why Don’t We All Have the Same Microbiome?

Whenever we are trying to live a healthy lifestyle, our bodies will go through so many changes. When we get rid of the bad stuff that is causing us problems and the beautiful thing start taking effect in what we put in our bodies. We, as humans, have different body structures and body types that are way different. Some people lose or gain weight differently. When other people exercises, they go at their own pace, and several factors influence the bacterial composition in taxa type and abundance. These factors include:
- host phenotype, such as age, gender, body mass index (BMI)
- lifestyle
- immune function
- geographical belonging and environmental factors
- use of antibiotics, drugs, and probiotics
- DIET
Moreover, long-term dietary habits have been shown to play a crucial role in creating an inter-individual variation in microbiota composition.
Manipulating the Microbiome: Key Terms
Here are some key terms to remember when we are talking about the microbiome.
- Stability: resistance to change and the ability to maintain homeostasis.
- Resilience: capacity to return to homeostasis after disturbance.
- Diversity: DIVERSE microbiomes are more stable and more resilient (to antibiotics); more resistant to foreign invasion (pathogens).
- Relative Abundance: Even ‘good’ bacteria can be too abundant without balance from symbiotic species; the presence of ‘bad’ bacteria is not necessarily always harmful if enough ‘good’ are there to balance.
- Colonization Resistance: The capacity of the microbiome communities to resist new colonization by pathogens and other transients.
- This is a KEY factor for preventing GI infections; but also explains why probiotics are not always practical.
- Our COMMENSAL microbiome is our first line and of defense
- Microbial depletion: Infection; Antibiotics; Toxins/Chemicals; Stress
- Restore balance/” reseeding”: (the term “reinoculate” is not really correct) Probiotics; Fermented foods; Prebiotics/Polyphenols.
Advantages to DNA Testing

For many practitioners, measuring microorganism DNA allows for:
- Detection of a more diverse collection of microorganisms, (more genus and species, particularly anaerobic species)
- They can measure at the species and subspecies level
- They have a much better snapshot of dysbiosis and diversity
- Have better accuracy of resultsMuch faster turnaround time and much less expensive
- Concept of “epigenetics.”
However, DNA is DNA-dead or alive whenever practitioners are looking at a patient’s DNA structure. Culture Technology is still considered “gold standard” but has several limitations. They are trying to culture anaerobic bacteria, but some of the most important bacteria are anaerobic commensals. There is a limited detection of several microorganisms, but it’s usually genus level only. Microorganisms can grow and/or die in transit and what’s measured in the culture dish is not always 100% indicative of the sample at the time of collection; the environment can morph while in transit to the lab and changes in pH etc.
Important Groups
These are some of the microbiomes that are very functional to our bodies and what parts do they play.
Commensals

This microbiome provides the host with essential nutrients and contains Aerobic and Anaerobic microbiomes.
- Aerobic (survives better in oxygenated environments; less prevalent in the colon, however, some are considered ‘obligate anaerobes’). They are:
- Lactobacillus
- Bifidobacterium
- Bacillus
- Anaerobic (more likely to be found colonizing the distal colon due to limited oxygen). They are:
- Clostridia
- Akkermansia
Lactobacillus and Bifidobacteria
These two are the most well-researched genus of bacteria. They are widely available in commercially available probiotic products.

- Lactobacillus are:
- lactic-acid forming bacteria
- Form biofilms which allow surviving harsh/low pH conditions (stomach acid)
- Helps maintain the integrity of the intestinal barrier
- Abundant in probiotics/fermented foods

- Bifidobacteria are:
- One of the first bacteria to colonize the gut after birth
- Aids in digestion, reducing inflammation, and stimulation of immune cells
Bacillus

These are spore-forming bacteria. They form spores in harsh environments which makes them more resilient, heat-stable, and have better viability in the gastric environment. But they may have better efficacy as probiotic therapy in SIBO population. These are in another category of commercially-produced probiotics beyond the standard Lactobacillus and Bifidobacterium.
In the health world, known as “Soil Based Probiotics.” They are very prominent in the environment and their primary role in immunomodulation; stimulation of the immune system. They are a production of GALT-Gut Associated Lymphoid Tissue and are known to be significant players in the production of B Vitamins and Vitamin K2 in the gut known as Bacillus subtilis
Clostridia

These are a major anaerobic group of commensals. They comprise 10% to >50% of the microbiome and are critical for the health of the gut barrier and intestinal lining, and barrier integrity. These are essential producers of butyrate (SCFA) and secondary bile acids. They also thrive on a high and diverse fiber diet, grape, and red wine polyphenols such as Blautia, Butyrivibrio, Eubacterium, Faecalibacterium prausnitizi, Roseburia, Ruminococcus, etc. However, there are usually no probiotic supplements to directly increase the abundance of clostridia.
Akkermansia

These microbiomes make up 1-3% of a healthy microbiome, and they help maintain the health and integrity of the mucosal barrier.
- Akkermansia muciniphila = mucin lover
They also help with reducing inflammation and may impart protection of inflammatory bowel diseases. These microbiomes are keystone species that are highly correlated with higher microbiome diversity.
Proteobacteria

This is a PHYLUM category of bacteria. This microbiome contains gram-negative and all bacteria that carries an LPS. This group includes plenty of beneficial bacteria but also contains several pathogens that tend to thrive in pro-inflammatory condition.
Gram (+) vs Gram (-) Bacteria

These two types of bacteria are in our bodies as they have very different functions that can either protect or disrupt our gut.
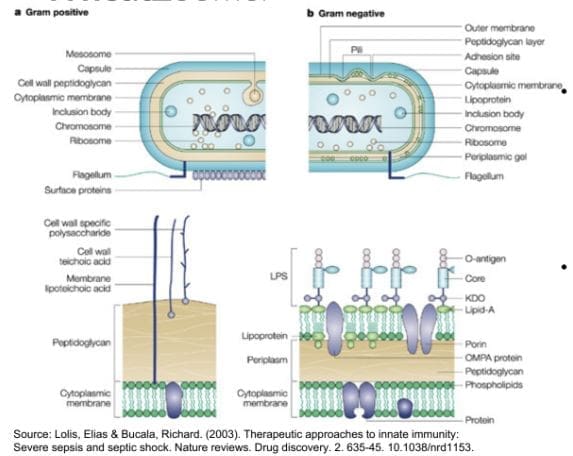
- Gram-Positive (+) contains:
- Peptidoglycan
- Lipoteichoic acid
- Gram-Negative (-) contains:
- LPS as a component of their cell wall
- LPS is a very powerful ENDOTOXIN- a known contributor to induce significant inflammation and potent immune response
- LPS antibodies are measured on Vibrant Wellness Wheat Zoomer/Intestinal Permeability Panel
However we can’t generalize Gram (-) as “bad” or Gram (+) as “good” or vice-versa, but we can control it with the Zoomers test.
LPS(Lipopolysaccharide)
In the last article, we mentioned them briefly, but here is a refresher on what theses microbes do. They are a fat/sugar molecule that lines the gram-negative bacteria inside the gut, and they protect those bacteria from bile salts. They are present inside the gut lumen under normal physiological conditions, and they usually should not enter the bloodstream. But if it does open in the blood then…
- 1) LPS antibodies are created-tagged as “non-self.”
- 2) Indication of intestinal permeability.
- 3) triggers multiple inflammatory cascades = ENDOTOXEMIA
- 4) Can help differentiate if leaky gut is happening between cells or through cells (or both), which are Transcellular vs. Paracellular pathways
Conclusion
These are the microbiomes that are in our body and how each of them plays a role to make our bodies healthy. We here at Injury Medical Clinic, do talk with our patients about what goes on in their bodies. We inform them on how to take care of themselves through the means of functional medicine. This is part one of a three-part series since tomorrow we will be discussing the roles of polyphenols in the Microbiome balance.
Post Disclaimer *
Professional Scope of Practice *
The information herein on "The Microbiome Functions and Functional Medicine Part: 1 El Paso, Texas" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Our information scope is limited to Chiropractic, musculoskeletal, physical medicines, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somatovisceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and/or functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez, DC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, RN*, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807, New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Florida
Florida License RN License # RN9617241 (Control No. 3558029)
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Presently Matriculated: ICHS: MSN* FNP (Family Nurse Practitioner Program)
Dr. Alex Jimenez DC, MSACP, RN* CIFM*, IFMCP*, ATN*, CCST
My Digital Business Card



