Physical Therapeutics for Herniated Discs | El Paso Chiropractor
Physical therapy plays a part in herniated disc recovery. Its methods not only offer you immediate pain relief, but they also teach you how you can condition your body to prevent further injury.
The discs are pads that serve as “cushions” between the vertebral bodies that serve to minimize the impact of movement on the spinal column. Each disc is designed like a jelly donut with a central softer component (nucleus pulposus).
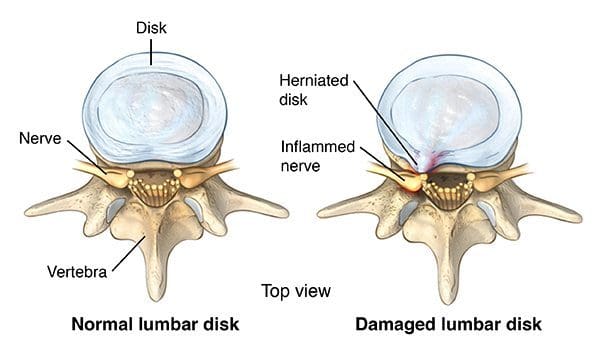
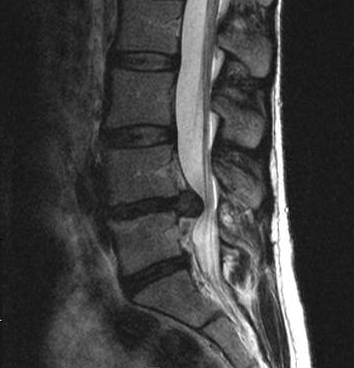
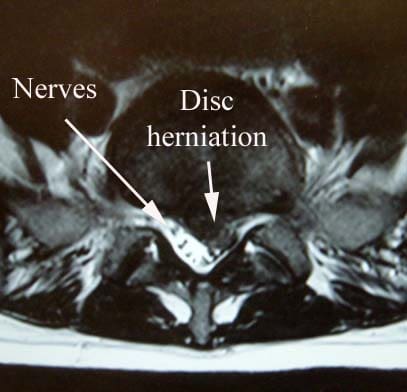
As the disc degenerates from age or injury, the softer central portion can rupture (herniate) through the surrounding outer ring (annulus fibrosus). This abnormal rupture of the central portion of the disc is referred to as a disc herniation. The most common location for a herniated disc to occur is in the disc at the level between the fourth and fifth lumber vertebrae in the low back.
You will find a variety of physical therapy techniques, such as passive treatments, which help relax your body and include deep tissue massage, hot and cold therapy, electric stimulation (eg, TENS), and hydrotherapy, among others.
Your physical treatment program will usually begin with passive remedies. But once your body heals, you will start active treatments that strengthen your body and protect against additional pain. Your therapist will work with you to develop a strategy which best suits you.
Table of Contents
Passive Physical Treatments for Herniated Discs
Deep Tissue Massage: There are more than 100 kinds of massage, but deep tissue massage is an ideal option when you’ve got a herniated disc because it uses a lot of pressure to ease deep muscle tension and spasms, which develop to stop muscle movement at the affected place.
Hot and Cold Therapy: Both hot and cold therapies offer their own set of advantages, and your physical therapist may alternate between them to get the best outcomes.
Your physical therapist may use heat to increase blood flow to the target region. Blood helps by delivering nutrients and additional oxygen cure the area. Blood also removes waste byproducts.
Conversely, cold therapy (also called cryotherapy) slows circulation. This decreases inflammation, muscle spasms and pain. Your physical therapist may put an ice pack give you an ice massage, or use a spray known to cool tissues.
Hydrotherapy: As the name implies, hydrotherapy involves water. As a passive therapy, hydrotherapy may involve sitting in warm shower or a bath. Hydrotherapy gently relieves pain and relaxes muscles.
Transcutaneous electric nerve stimulation (TENS): A TENS machine utilizes an electrical current to stimulate your muscles. It isn’t painful, although it seems extreme. A electric current is sent by electrodes to key points on the neural pathway. TENS reduces muscle spasms and is generally believed to activate the release.
Traction: The goal of traction is to decrease the effects of gravity to the spine. The aim is to cut back the disk herniation, by pulling the bones apart. The analogy is similar to a flat tire “disappearing” when you place a jack under the car and take strain off the tire. It can be carried out in the lumbar or cervical spine.
Active Physical Treatments for Herniated Discs
Active remedies help address flexibility, posture, strength, core stability, and joint motion. An exercise program may also be prescribed to achieve results. This will not just suppress recurrent pain but may also benefit your health. Your therapist may work with you to develop a schedule based on your diagnosis and health history.
Core equilibrium: Many people don’t realize how important a strong heart is to their spinal health. Your core (abdominal) muscles help your back muscles support your spine. It puts pressure when your heart muscles are weak. Your physical therapist may teach core to you.
Flexibility: Learning appropriate stretching and endurance techniques will prepare one for aerobic and strength exercises. Flexibility helps your body move simpler by warding off stiffness.
Hydrotherapy: Compared to just sitting in a hot bath or bath like its counterpart that is passive, active hydrotherapy can demand water to help condition your body without unnecessary strain.
Muscle strengthening: Strong muscles are a great support system for your backbone and better handle pain.
Your physician will teach you ways to condition and strengthen your back to help prevent future pain. So that you realize how to best treat your symptoms, you may learn fundamentals. The aim is that you develop the knowledge to maintain a way of life.
It is essential that you understand how to exercise and condition your back following the formal physical therapy ends. You won’t appreciate its results, if you don’t implement the lessons you learned during physical therapy. You might prevent additional disc pain, by taking care of your back on your own.
The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss options on the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 . 
By Dr. Alex Jimenez
Additional Topics: Sciatica
Lower back pain is one of the most commonly reported symptoms among the general population. Sciatica, is well-known group of symptoms, including lower back pain, numbness and tingling sensations, which often describe the source of an individual’s lumbar spine issues. Sciatica can be due to a variety of injuries and/or conditions, such as spinal misalignment, or subluxation, disc herniation and even spinal degeneration.

TRENDING TOPIC: EXTRA EXTRA: New PUSH 24/7®? Fitness Center
Post Disclaimer *
Professional Scope of Practice *
The information herein on "Physical Therapeutics for Herniated Discs | El Paso Chiropractor" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Our information scope is limited to Chiropractic, musculoskeletal, physical medicines, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somatovisceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and/or functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez, DC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, RN*, CCST, IFMCP*, CIFM*, ATN*
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807, New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Florida
Florida License RN License # RN9617241 (Control No. 3558029)
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Presently Matriculated: ICHS: MSN* FNP (Family Nurse Practitioner Program)
Dr. Alex Jimenez DC, MSACP, RN* CIFM*, IFMCP*, ATN*, CCST
My Digital Business Card